Irony is spending 20 years wondering why your students sometimes struggle to be quiet, and suddenly, in one week, realizing how insanely difficult it is to be silent, AND, that it’s likely your need to talk constantly is part of the reason WHY you went into teaching in the first place!
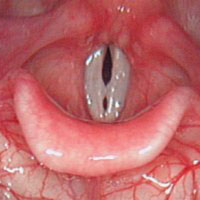
Last Friday, March 3rd, this ugly thing was taken off my vocal cords.

And they, like so many other parts of my body, now boast scars.

So, I set up for a few weeks out of work, and a week of required silence. I never actually thought I was ready, which is a good thing. Because I wasn’t.
I do poorly on twitter, Rarely could I get out what I need in 140 characters or less. Absolute silence involved my cell phone in hand at all times. A few times the thing almost learned to fly, as the fingers, and auto-correct could not keep up with my brain. But, life lesson number, oh, I don’t know, 4 or 5, teaches us that life goes on around us. Ready or not. Even when you have to watch and not participate.
There have been many times since March 3rd I’ve been grateful that thought bubbles do not appear above my head.
On the 9th I headed to the city for my follow-up. After learning the pathology was benign, and read only “polyp,” I was relieved. The doctor was pleased with the initial healing and told me I could begin to use my voice. Slowly. He said 5 minutes an hour. That sounded high, based on what the voice therapist had told me in the fall, but I was grateful. I used the first 5 minutes up asking him questions.
I wanted to know whether this was connected to Cowden’s Syndrome. I wanted to know if it was likely to recur, if I needed vocal therapy, and when my follow-up would be.
Apparently, kind as he is, he could communicate on Twitter much more efficiently than I.
Cowden’s Syndrome? I don’t know. There’s not a lot of literature. This type of polyp is usually a traumatic event, something you’d remember. But, you don’t. And it grew really fast. I’m not sure.
Recurrence? Maybe. Depends how it came to be. Be careful with your voice.
Vocal Therapy? Suggested. Start on the 13th. (Whew… THAT I now KNEW I needed.)
Follow up – April 13th, a few days before I am scheduled to teach my first class post-operatively.
He was an outstanding surgeon. Matter-of-fact. Thorough. Efficient. But, I’ve known enough surgeons now to know, they don’t play with why. They just fix it and move on. He will “doctor” me, to the point that he will follow-up, and hopefully watch NOTHING ever grow there again. But, in reality this is now just another vulnerable spot on this PTEN mutated body. Because, I would stake certainty that it’s connected. There just aren’t that many coincidences in life.
So I left Thursday feeling good. I got 5 minutes an hour! I tried out my voice in the car. I tried it out at home. And then, I picked up my daughter at school, and I was so excited to talk to her, I easily let the conversation surpass 15 minutes. oops.
Later when I spoke to my husband I was well past 10 before I stopped.
This 5 minutes and hour thing was not for the faint of heart!
Sometime Friday I decided that stopping at 5 minutes was, nearly impossible for me to regulate. It was quite possible I could lose my mind.
And then I texted the voice therapist to set up my appointments for this week. And I mentioned the 5 minutes. And that I randomly out of nowhere had vomited for 20 minutes that morning. And her words were crystal clear. “DO NOT SPEAK AGAIN UNTIL I SEE YOU”
Sucker Punch
I went from a poorly managed 5 minutes back to a feeble attempt at silence.
I failed.
I spent 2 full days at a swim meet at with my girl. 7 hours each day away from home. I got to rest my voice, except when I felt compelled to tell her how proud I was. Or to wish her luck. Or to just chat… a little.
Some people really love chocolate. Me, I don’t mind chocolate, but I LOVE to talk.
We sat in therapy today and I got exercises for volume and pitch… all ironic because I struggle to tell the difference, but I’m an overachiever, so I try to do well. I sound like a complete loser, but I imagine it’s the same as me attempting something that requires coordination, like kick-boxing, or yoga. My poor vocal cords may not stand a chance.
6 exercises, 5 times each. Repeat 4x a day. And during those 4 hours DON’T SPEAK at all.
The revised schedule she gave me had 3 minutes an hour till Friday. Then, we’ll entertain 5 minutes again.
Tonight I pulled back into my office. To be silent I must be alone. I put some “breathe” into my diffuser, and tried to get my thoughts together.
Then I realized they ARE together. I just have no place to put them.
Tomorrow the house will be full for the snow day. Normally this would make me very happy. Tomorrow it is likely to make me a hermit.
Grateful the voice works. Grateful I tend to heal well…. But, some days
#beatingcowdens
is a real trip!